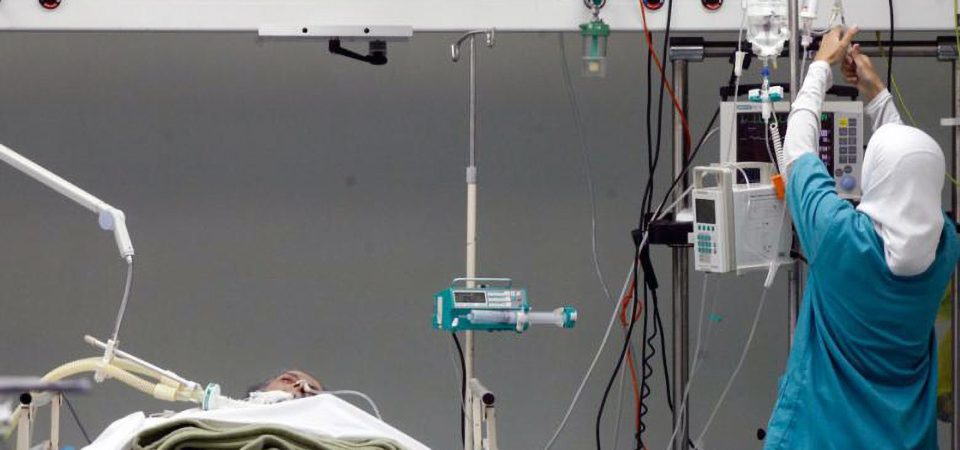
While the Lebanese healthcare system has been resilient in navigating through previous phases of political instability, the stress experienced by it during the current period of anti-government protests is challenging on many levels.
In a press release issued on December 10, 2019, Human Rights Watch underscored the impact of the financial crisis on the right to health and urged both the Finance Ministry to disburse funds owed to hospitals and the Central Bank to develop clear and cohesive regulations for businesses.
Less than a month later, the head of the Syndicate of Private Hospitals, Sleiman Haroun, told local media that hospitals have been unable to perform many surgeries due to their inability to pay for medical supplies and spare parts for medical equipment.
The basis for the effectiveness of Lebanon’s collaborative governance networks is in technical capacity, strategic intelligence, transparency, and consensual leadership. The fabric of these networks, and the services they offer, is rendered sensitive by the current state of the economy.
On January 10, 2020, Hussain Isma’eel, president of the Medical Committee at AUBMC, wrote a commentary on the healthcare crisis in Lebanon and highlighted the importance of transparency, as well as the few steps taken towards the positive direction.
A relevant study published in 2012 sheds light on a topic that should be valuable to any future austerity measures: the role of informal politics and clientelistic networks in access to healthcare.
Informal politics aggravate healthcare inequalities
Informal practices, whereby access to social services is used as a deliberate strategy by politicians and political parties to gain and reward support, can affect access to healthcare and exacerbate health inequalities in the population.
In the context of weakened state institutions, the public sector plays a minimal role in ensuring social protection while non-state actors (such as political parties and NGOs) predominate in the welfare regime. The 2012 study by Bradley Chen and Melani Cammett looked at the role of informal politics in influencing access to healthcare at the individual level in Lebanon.
The authors conducted in-depth interviews with 175 officials in the Ministries of Public Health and Social Affairs, NGO representatives, officials from political parties and religious institutions, and local journalists and researchers. They also interviewed 135 Lebanese citizens from diverse religious backgrounds to gather information on their experiences in accessing health care and other forms of social assistance. Surveys were furthermore collected from 1789 households.
Their results suggested that individuals with higher political activism have better access to health services than others because of their likelihood of receiving financial assistance. As such, informal, micro-level political institutions can have an important impact on healthcare access and utilization, with potentially detrimental effects on the least politically connected.
Their analysis highlights the role of informal institutions and individual or household level exchanges in mediating access to healthcare and point to a gap between de jure and de facto social rights: Although needy citizens are eligible for public coverage of treatment for certain diseases and for hospitalization, in practice their access to these “entitlements” is mediated at least in part by politicians and political organizations that exert influence over relevant agencies in Lebanon.
The authors also point out that new health inequities can appear given discriminatory access to medical care on the basis of political participation at the individual and household levels.
In his commentary, AUBMC’s Hussain Isma’eel mentions the following about the current situation “The worst is: not having clear and transparent ethical guidance for health policy austerity-driven decisions. This will further aggravate the economic challenges by introducing absence of trust and scepticism regarding egalitarian allocation of resources”. Where do informal politics stand in terms of utilitarianism and transparency?